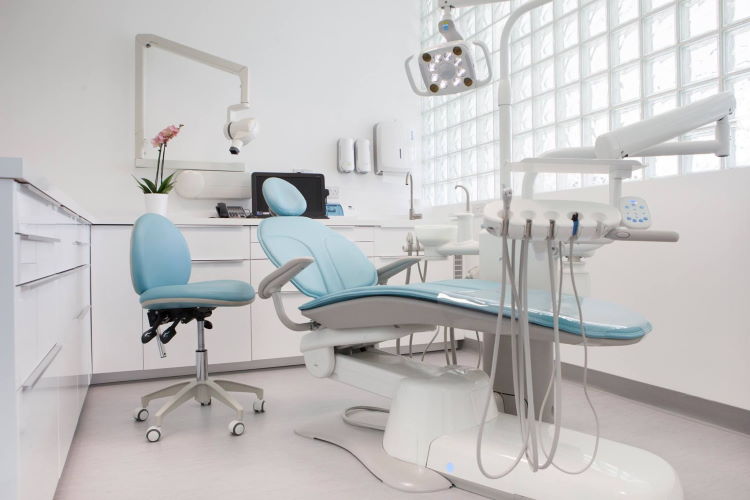
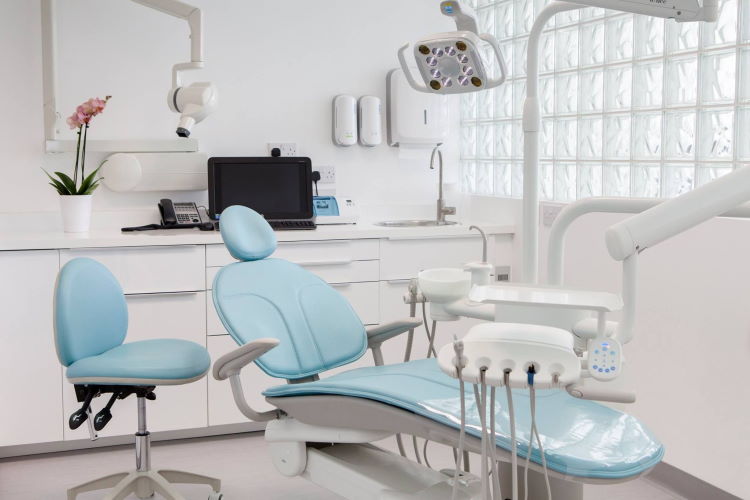
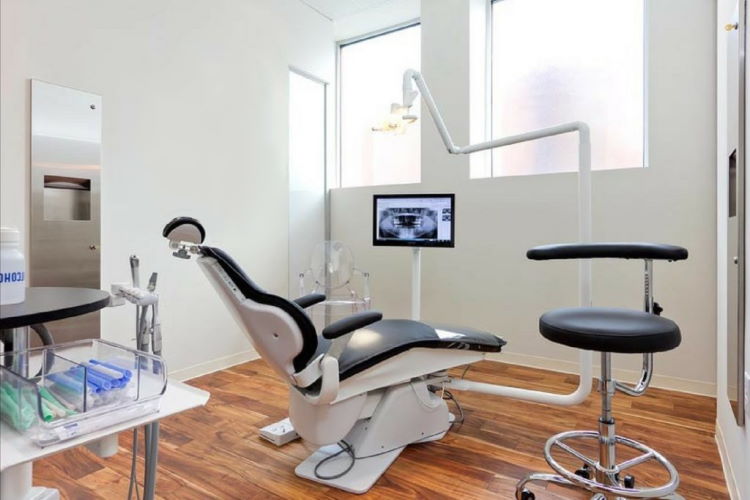
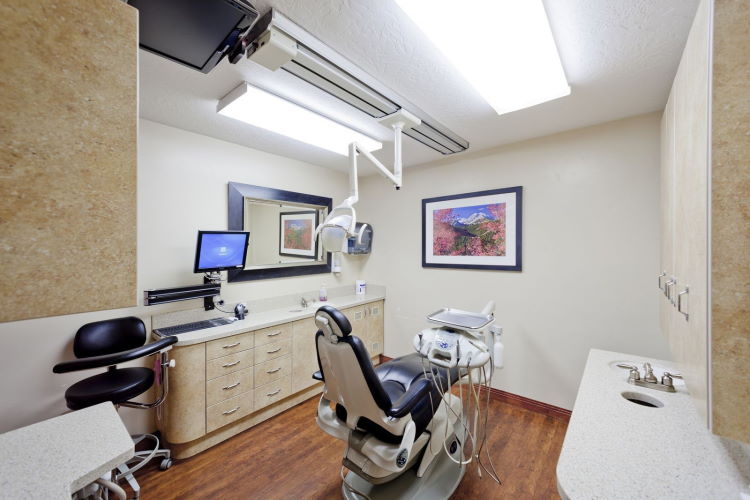




Welcome to Dr. Madhvi’s Dental Clinic, located in New Delhi, India. We are a team of dentists, doctors and surgeons with over 16 years of experience in all dental treatments.




We at Dr. Madhvi’s Dental Clinic, are a team of well-qualified doctors, surgeons and assistants. We use the latest equipment and material in the treatments. And we keep ourselves updated with the latest innovations in dentistry.
Dr. Madhvi Nagpal and her team have been practicing dentistry in New Delhi, India for the last 16 years. She has treated over 100 thousand patients during her practice.

We strongly believe that everyone deserves medical treatment irrespective of affordability. Therefore, we offer all the latest dental treatments at a very low price. We are also involved in various community services to make people aware of oral hygiene and affordable dental care.

You can contact us anytime to get a price estimate of your dental treatment. We also are available on live chat on WhatsApp / Facebook / Viber at +91.9810554230 (India)





